You felt your leg pulse. Then you noticed it again. Now you’re here.
Welcome to the club. Basically every adult winds up Googling this at some point.
Most leg throbbing turns out to be nothing. Just a normal artery doing its job while you happened to be paying attention. Some of it isn’t nothing.
The point of this guide is to help you tell the two apart. Without panicking, and without dismissing something that actually deserves a phone call.
What follows covers every realistic cause: vein problems, artery problems, the non-vascular stuff most articles skip, and the small list of scenarios where you should put the phone down and head to an ER.
Medical claims here lean on current CDC, NIH, and AHA data. None of it replaces a doctor. It should make you a sharper patient when you talk to one.
Quick answer: why is my leg throbbing?
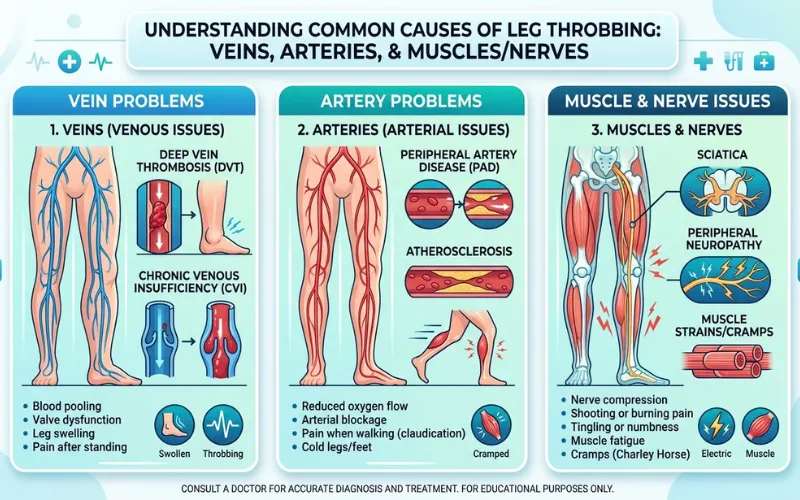
Three buckets.
Vein-related: chronic venous insufficiency, varicose veins, or rarely a clot. Artery-related: peripheral artery disease, sometimes an aneurysm. Non-vascular: muscle twitches, dehydration, a pinched nerve, or just hearing your own pulse in a quiet room.
A pulse you can feel is not, by itself, an emergency.
A pulse plus sudden swelling, a hot or red leg, or shortness of breath is.
If you’ve got 30 seconds, jump to the triage table. If you’ve got a few minutes, the rest is worth reading.
What throbbing actually feels like
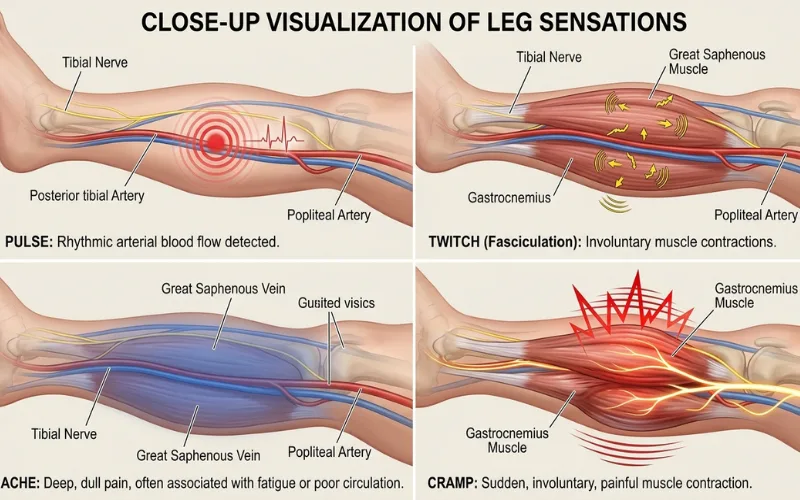
People describe it different ways. The description matters because it points to different causes.
- Common patterns and what they tend to mean:
- A rhythmic pulse that matches your heartbeat. Usually vascular.
- A buzzing or fluttering. Usually nerve or muscle.
- A heavy, achy throb that gets worse by evening. Classic vein problem.
- A sharp throb with pain that came on fast. Could be a clot, especially in one leg.
- A localized “twitch” that comes and goes. Almost always a muscle fasciculation.
If your leg feels like it has its own heartbeat but there’s no pain, no swelling, and no skin change, you’re likely feeling a normal artery.
The femoral runs through your thigh. The popliteal sits behind your knee. The posterior tibial passes near the inner ankle. Any of them can be felt, especially in lean people, lying still, or when you’re really paying attention.
“Probably normal” isn’t the same as “definitely normal.” Read on.
Is it normal to feel a heartbeat in your leg?
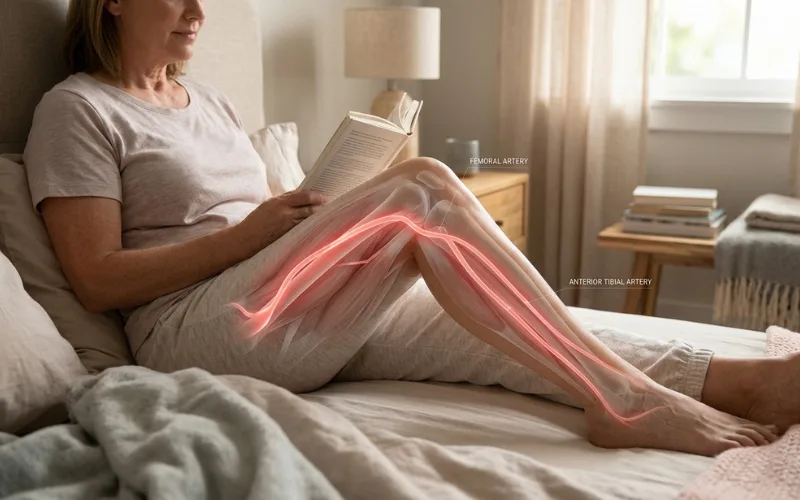
Sometimes, yes.
Common situations where the pulse becomes noticeable:
- After exercise, when your heart rate is up.
- Lying flat in a quiet room.
- After a hot shower or bath.
- During pregnancy, when blood volume rises by 30 to 50 percent.
- When you’re anxious, jittery, or wired on caffeine.
- If you’re naturally thin.
Pulsing that comes and goes, fades quickly, and isn’t paired with pain or swelling is almost always benign pulse awareness. Bodies have arteries. Sometimes you notice them.
It’s a different conversation when the pulsing is new, sticks around for weeks, lives in only one leg, gets worse, or shows up with the warning signs in the next section.
When to go to the ER (self-triage)
Use this table to decide.
| What you’re feeling | What it might be | What to do |
| Throbbing plus sudden one-leg swelling, warmth, redness, tenderness | Possible deep vein thrombosis | Same-day ER or urgent care |
| Throbbing plus chest pain, shortness of breath, coughing blood | Possible pulmonary embolism | Call 911 |
| Severe throbbing plus a cold, pale, numb foot; no pulse | Possible acute limb ischemia | Call 911 |
| Pulsating mass behind the knee or in the groin | Possible aneurysm | Same-day vascular evaluation |
| Calf pain that starts when you walk and stops at rest | Possible peripheral artery disease | Schedule with primary care or vascular specialist |
| Heavy ache that’s worse at night or after long standing | Possible chronic venous insufficiency or varicose veins | Schedule a vein specialist visit |
| Brief twitch in one spot, no pain, comes and goes | Likely benign | Watch and wait; see a doctor if it persists |
The shorthand: new, one-sided, persistent. Get it checked.
Vein-related causes
Vein problems are the most common reason patients walk into a vascular clinic asking about leg throbbing. Here’s why.
Veins move blood back to the heart against gravity. They rely on one-way valves and the squeeze of your calf muscles. When that system fails, blood pools, pressure rises, and the legs throb.
1. Chronic venous insufficiency (CVI)
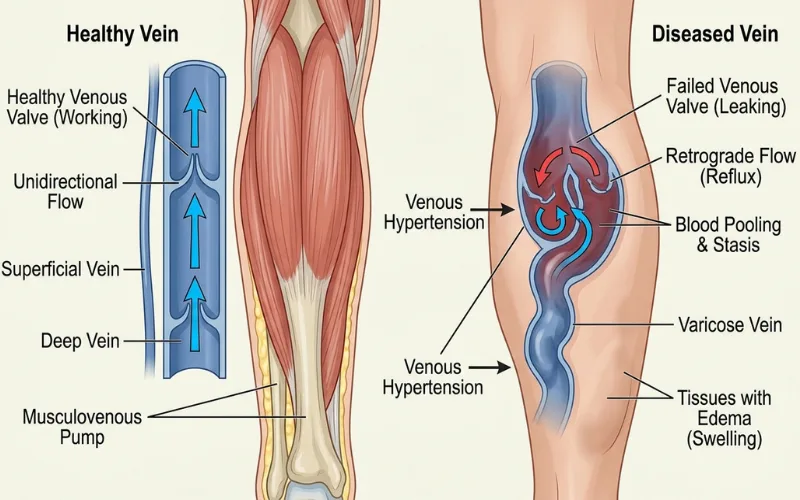
CVI is the umbrella term for vein valves that no longer close properly. Blood leaks backward. Pressure builds. You feel it.
Roughly 25 million U.S. adults have CVI, with about 6 million at advanced stages, per peer-reviewed estimates. The NIH-affiliated StatPearls database puts the cost of care at nearly $500 million a year, with around 150,000 new diagnoses annually.
What CVI feels like:
- Throbbing or aching that worsens by evening.
- Heaviness or “tired legs” after standing.
- Ankle swelling that backs off when you elevate.
- Itching, burning, or restless legs at night.
- Visible varicose veins or skin darkening near the ankles.
If both your legs throb, it’s worse the longer you’re upright, and putting your feet up actually helps, CVI is on the short list.
2. Varicose veins
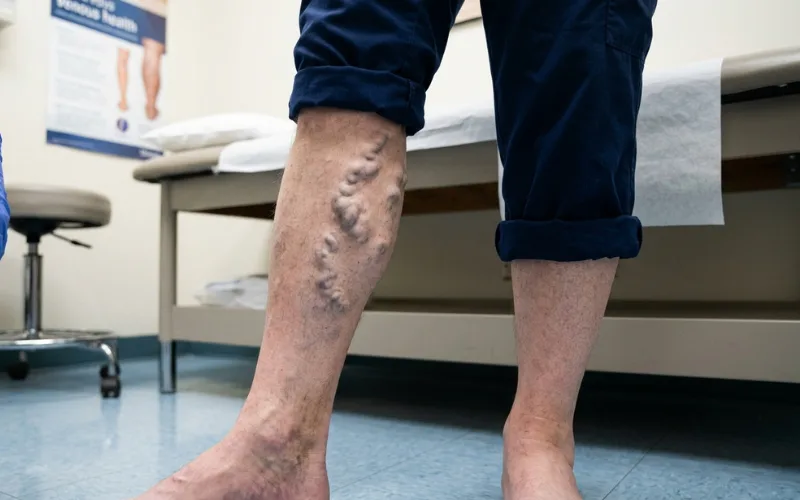
Varicose veins are the bulging, ropy, blue-purple veins everyone associates with vein trouble. They form when valves fail and surface veins stretch under the pressure of pooled blood.
Population studies cited in PubMed show varicose vein prevalence ranges widely. Under 1 percent to 73 percent in females. 2 to 56 percent in males. The takeaway: extremely common, especially with age, pregnancy, and standing-heavy jobs.
A throb directly over a visible varicose vein, especially after a long day, fits the picture. The vein isn’t pumping arterial blood. You’re feeling pressure from pooled venous blood plus tissue irritation around it.
3. Deep vein thrombosis (DVT)
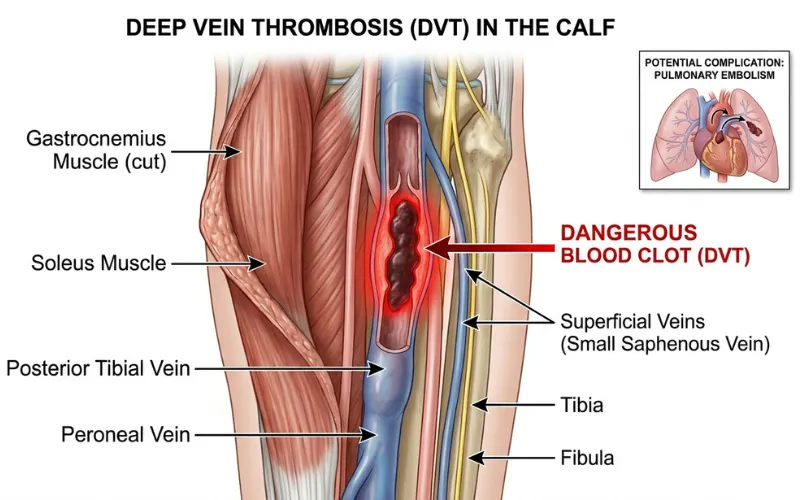
This is the one you don’t want.
A DVT is a clot in a deep leg vein. If part of it breaks off and travels to the lungs, it becomes a pulmonary embolism, which kills people.
CDC data: as many as 900,000 Americans are affected by DVT or PE each year. Sudden death is the first symptom in roughly 25 percent of pulmonary embolism cases. Annual U.S. deaths from venous thromboembolism: 60,000 to 100,000.
Watch for:
- Throbbing or cramping pain in one leg, not both.
- Sudden swelling, often in the calf.
- Warmth and redness.
- Tenderness when you press on the calf.
- A faintly bluish or discolored look to the skin.
Risk goes up after surgery, long flights, hospital stays, pregnancy, hormonal birth control, cancer, and inherited clotting disorders. If your throb came on suddenly in one leg and the leg is swollen or warm, treat it as urgent.
4. Superficial thrombophlebitis
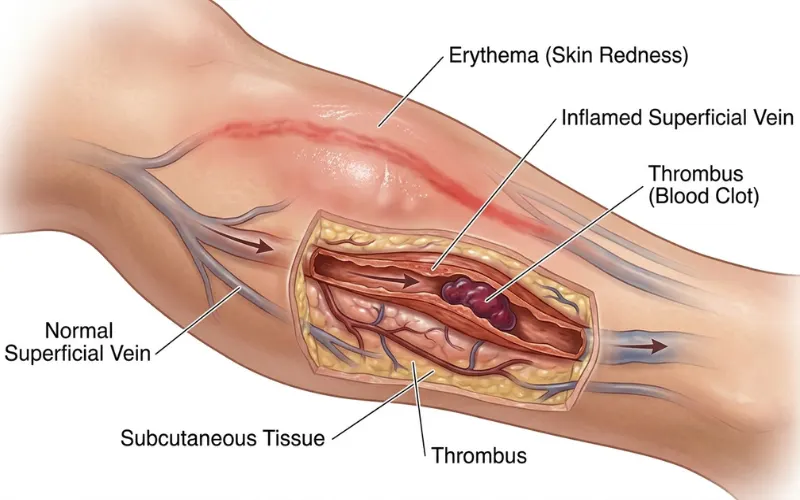
A clot in a vein near the skin. It feels like a tender, hard, warm cord you can sometimes trace with your finger.
Less dangerous than a DVT. Still worth a visit, especially if it’s spreading up the leg or near the groin.
Artery-related causes
Arteries carry pressurized, oxygen-rich blood out to the legs. When they narrow or weaken, the symptoms differ from vein problems.
5. Peripheral artery disease (PAD)
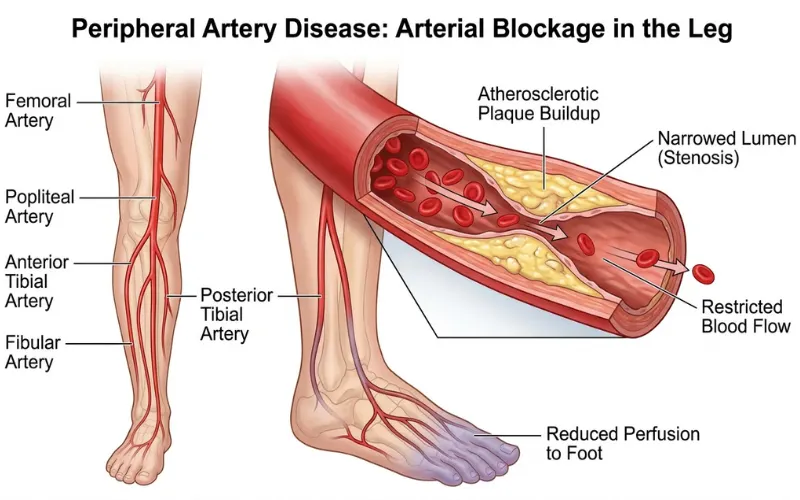
PAD is plaque buildup in leg arteries. About 8 million Americans over 40 have it, per the NHLBI. Globally, more than 200 million.
Up to 4 in 10 people with PAD don’t feel any leg pain at all. The CDC and AHA both confirm this stat.
When PAD does cause symptoms, the classic one isn’t really throbbing. It’s intermittent claudication: a cramping calf pain that shows up when you walk and goes away when you rest.
Some patients call it a deep ache or a throb. The pattern is what counts. Pain tied to exertion, gone with rest.
Other PAD signs:
- One foot or leg colder than the other.
- Pale, bluish, or shiny skin on the lower leg.
- Hair loss on the toes or shins.
- Sores or wounds that heal slowly or not at all.
- Weak or absent pulses in the foot.
PAD is what most people mean when they say “clogged arteries in the legs.” Full warning sign list further down.
6. Popliteal artery aneurysm
A weakened, bulging spot in the artery behind the knee. Uncommon. Worth catching.
If you can feel a distinct pulsing lump behind your knee, get a same-week vascular evaluation. These can clot or send debris downstream and threaten the foot.
7. Acute limb ischemia
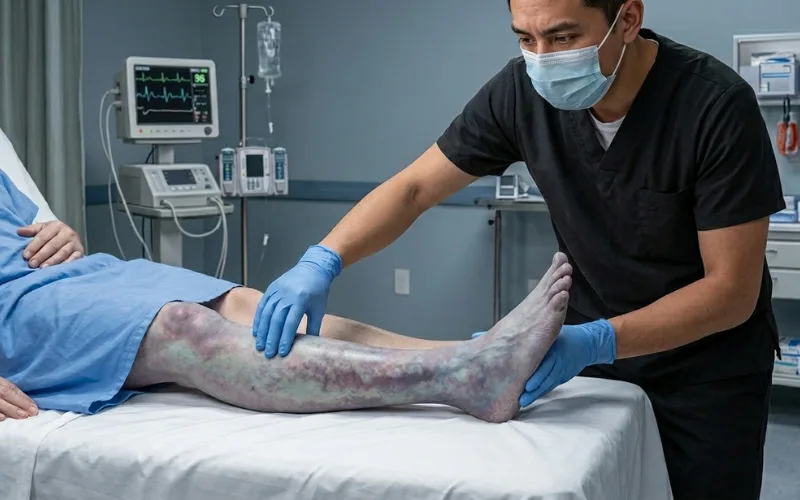
Sudden loss of blood flow to the leg. The leg goes pale, cold, painful, weak. Pulses disappear.
This is a 911 emergency. Without restored blood flow within hours, people lose limbs.
Non-vascular causes (often missed)
Most articles on this topic stop at veins and arteries. But plenty of patients with throbbing legs have neither.
8. Benign muscle fasciculations
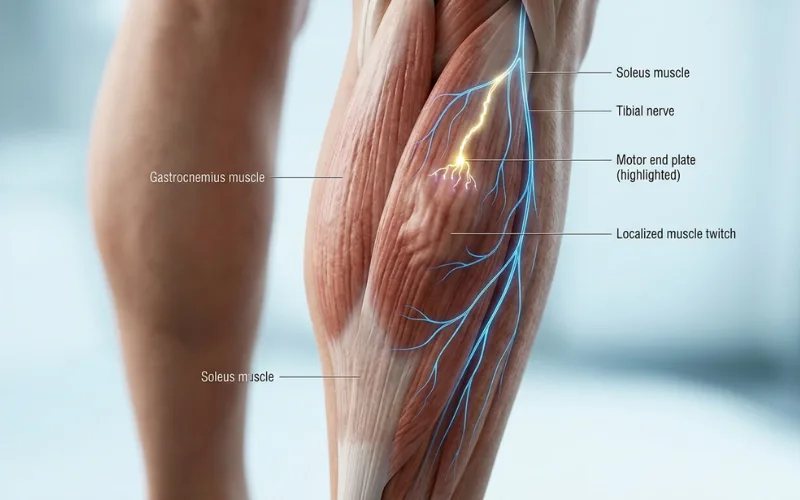
A fasciculation is a small, involuntary twitch.
Per the Cleveland Clinic, benign fasciculation syndrome causes frequent twitches without an underlying medical condition, typically at one site in one muscle at a time. Annoying. Harmless.
If you feel a small, localized “pulse” in your calf, thigh, or eyelid that comes and goes, that’s likely a fasciculation, not a vascular pulse. Triggers include caffeine, stress, fatigue, dehydration, and electrolyte issues.
The simple distinction: vascular pulses are rhythmic and match your heartbeat. Fasciculations are irregular and feel more like a flutter or flick.
9. Dehydration and electrolyte imbalance

Low magnesium, low potassium, plain old dehydration. Muscles get twitchy. The result can feel like throbbing.
Athletes who train hard and skip the water often notice this in their calves at night.
10. Pinched nerve or sciatica
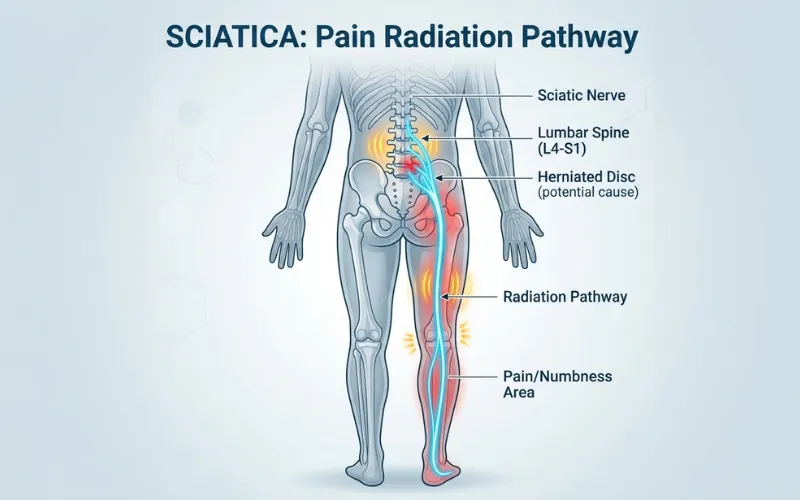
Lumbar nerve compression can radiate into the leg as burning, tingling, or “pulsing.” Nerve pain follows a specific path, like the lower back down the back of the leg, and doesn’t usually cause swelling or temperature differences.
If your throb runs in a stripe down the back of the leg and gets worse with certain back positions, sciatica is on the list.
11. Anxiety and heightened body awareness

When the sympathetic nervous system fires (stress, panic, caffeine), you become more aware of normal sensations. The pulse you ignored all day becomes alarming at 2 a.m.
Real, not “in your head.” Also not vascular disease. If a workup comes back clean and the throbbing matches stress patterns, anxiety management is the right path.
12. Pregnancy

Blood volume jumps during pregnancy. The uterus presses on pelvic veins. Hormones relax vein walls.
The result: more visible veins, more pulsing, sometimes new varicose veins.
Most pregnancy-related leg throbbing fades after delivery. But sudden one-sided swelling always needs evaluation. Pregnancy raises DVT risk too.
13. Restless legs syndrome (RLS)

RLS is an uncomfortable urge to move the legs, often described as crawling, throbbing, or pulling. Worst in the evening or at night. Better with movement.
It’s neurologic, not vascular. Often linked to iron deficiency.
14. Injury or muscle overuse

A bruised muscle, a hamstring strain, a hard workout, plain overuse. Inflammation throbs.
If swelling stays local to the injured area and the rest of the leg looks normal, rest, ice, and time generally fix it.
Vein vs. artery vs. non-vascular: telling them apart
Most people can narrow the source themselves with this comparison.
| Feature | Vein-related | Artery-related | Non-vascular |
| Timing | Worse end-of-day | Worse with walking, better at rest | Random, often at night |
| Location | Calves, ankles, often both legs | Calf, thigh, or buttock with walking | Localized to one spot |
| Sensation | Heavy, achy throb | Cramping, tight, burning | Twitch, flutter, “tic” |
| Visible signs | Varicose veins, ankle swelling, skin darkening | Pale, cold foot; hair loss; slow-healing sores | None |
| Relief | Elevation, walking, compression | Stopping the activity | Stretching, hydration, rest |
A vascular ultrasound can usually clarify the cause inside 30 minutes.
Why is my leg throbbing in one specific spot?
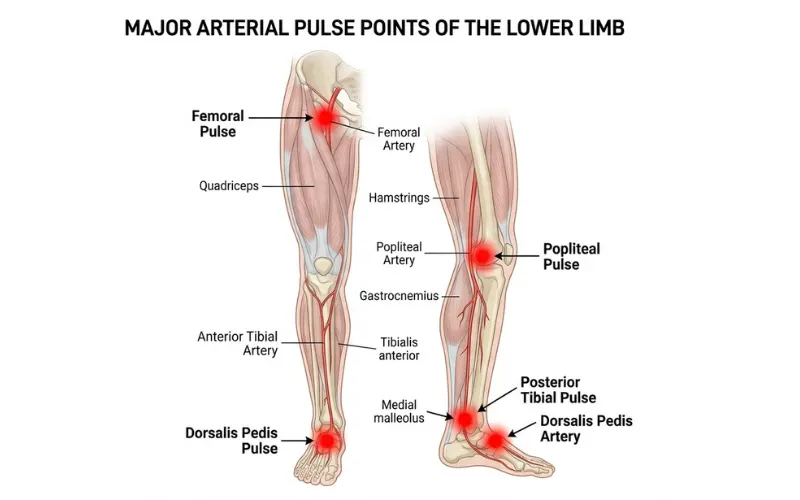
If the throb sticks to one location, the cause is usually local rather than systemic.
Common patterns:
- Behind the knee. Popliteal artery (normal in thin people) or, rarely, popliteal aneurysm.
- Inner thigh near the groin. Femoral artery pulse, varicose vein in the great saphenous vein, or pelvic congestion in some women.
- Calf. Gastrocnemius muscle fasciculation, varicose vein, or DVT (especially with pain and swelling).
- Top of the foot or inner ankle. Posterior tibial or dorsalis pedis artery pulse. Often nothing.
- Outer thigh above the knee. Surface veins or overuse from running and cycling.
A throb in one spot, no pain, no swelling, no skin change, is almost always benign. If it sticks around for weeks, get checked anyway.
Why is my leg throbbing when I’m lying down?

This question comes up a lot. Three reasons it happens.
When you lie flat, your heart isn’t fighting gravity, so pulses become more noticeable. Your sensory attention shifts to your body because there’s nothing else to focus on. And blood pooled in your lower legs from a day of standing starts redistributing.
Net effect: perfectly normal arterial pulses become loud.
Many patients only feel the heartbeat in their legs at night. Unless it comes with pain, swelling, or skin changes, this is almost always normal pulse awareness, sometimes amplified by anxiety or caffeine earlier in the day.
If the throb starts when you lie down and disappears when you sit up or walk, that pattern argues against anything serious.
Why is my leg throbbing after sitting too long?

Sitting compresses the veins behind your knees. Blood return slows. Pressure builds in the lower legs.
When you finally stand, the rush of blood flow can feel like throbbing or pulsing, especially in the calves. Long flights, long drives, desk jobs.
This is also when DVT risk rises. The CDC has documented elevated VTE risk after immobility lasting four hours or more. If you’ve been sitting a long stretch and develop calf pain plus swelling, don’t shrug it off.
Warning signs of clogged arteries in legs
One of the most-asked questions about throbbing legs. Here’s the full list, drawn from CDC and AHA guidance:
- Pain, cramping, or aching in the calf, thigh, or buttock when walking, gone with rest.
- One foot or leg colder than the other.
- Pale, bluish, or shiny skin on the lower leg.
- Slow-growing or thickened toenails.
- Hair loss on the lower leg or feet.
- Sores or ulcers on the feet that heal slowly or not at all.
- Weak or absent pulses in the feet (your doctor checks for this).
- Numbness or weakness in the leg.
- Erectile dysfunction in men, when the lower aorta or iliac arteries are involved.
The CDC notes the classic PAD symptom is leg pain with physical activity that improves with rest. But up to 4 in 10 people with PAD have no leg pain.
Screening matters if you’re over 65, over 50 with diabetes or smoking history, or have a strong family history.
The ankle-brachial index (ABI) test compares blood pressure in your ankle to the pressure in your arm. Takes 10 to 15 minutes. Cheap. Painless. Catches PAD long before symptoms get bad.
How doctors diagnose throbbing legs
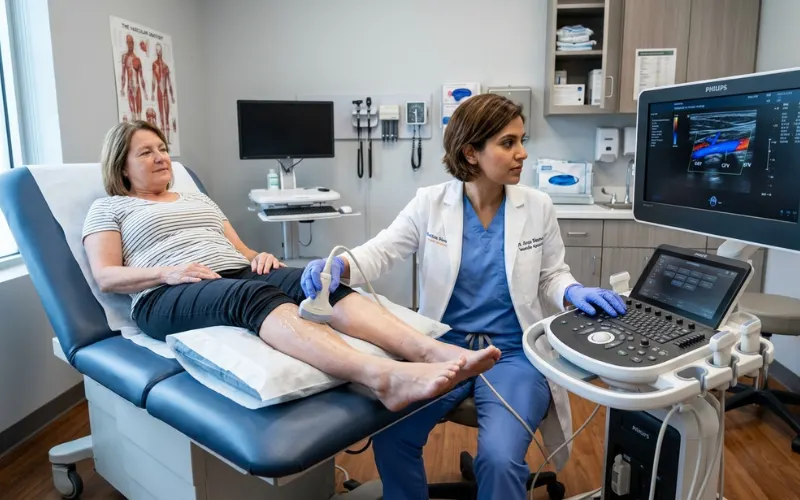
A vascular workup is faster and less invasive than people expect.
A typical visit involves:
- History and physical. Where the throb is, when it started, what makes it better or worse, your risk factors.
- Inspection. Looking for varicose veins, swelling, skin changes, ulcers, hair loss, color asymmetry between legs.
- Pulse check. At the groin, behind the knee, at the ankle and foot.
- Duplex ultrasound. The workhorse test for both vein and artery problems. Maps blood flow with sound waves. Catches DVT, valve failure, plaque, aneurysms.
- Ankle-brachial index. For suspected PAD.
- CT or MR angiography. When more detail is needed before a procedure.
Most patients leave the first visit with either a clear diagnosis or a plan to confirm one.
Home care that actually helps

If your throb is mild and you don’t have any red flags, conservative measures often resolve it.
- Walk. Calf muscles are the biggest natural pump for venous return. 30 minutes a day helps.
- Elevate. Above heart level. 15 to 20 minutes, two or three times a day. Pillows under the calves while you watch TV.
- Compression stockings. Knee-high, 15-20 mmHg or 20-30 mmHg. Not fashionable. They work. Many patients with venous symptoms feel less throbbing within days.
- Hydrate. Two to three liters of water a day. Cuts down on muscle cramping.
- Lose extra weight if it applies. Less weight, less pressure on lower veins.
- Move during long sits. Every 60 minutes, stand and walk for 2-3 minutes. Calf raises in your seat on flights.
- Skip very hot baths and saunas if you have varicose veins. Heat makes pooling worse.
- Easy on caffeine and alcohol in the evening if the throb is worst at night.
- Sleep and stress matter. Anxiety amplifies the signal you’re feeling.
If two to four weeks of consistent home care doesn’t budge it, get evaluated. Vein problems are easier to fix early.
Treatment options for vascular causes
When a doctor finds a treatable cause, current options include:
- Compression therapy and lifestyle changes. First-line for most CVI cases.
- Sclerotherapy. A chemical injection that closes small varicose and spider veins.
- Endovenous laser ablation (EVLA) or radiofrequency ablation (RFA). A thin catheter heats and seals failing veins from the inside. Office procedures with same-day recovery.
- Microphlebectomy. Tiny incisions to remove larger surface varicose veins.
- VenaSeal. Medical adhesive that closes the vein.
- Anticoagulation (blood thinners). For DVT. Usually 3 to 6 months minimum.
- Antiplatelet therapy, statins, supervised exercise. For PAD.
- Angioplasty, stenting, or bypass surgery. For severe PAD or limb-threatening ischemia.
Most vein and artery care has moved out of the hospital operating room and into outpatient clinics. Walk in, local anesthesia, walk out the same day.
How to prevent leg throbbing and vascular problems
The same boring list everyone has heard. Still works.
- Don’t smoke. Smoking is the single biggest modifiable risk factor for PAD and a major contributor to DVT and vein damage.
- Keep blood pressure under 130/80 mmHg.
- Keep LDL cholesterol low. Talk to your doctor about your target.
- Manage diabetes tightly if you have it.
- Move every day. Walking counts. Swimming and cycling are better.
- Maintain a healthy weight.
- After surgery or long flights, hydrate, walk early, wear compression if recommended.
If vein disease runs in your family, ask about earlier screening.
Frequently Asked Questions (FAQ’s)
Why does my leg pulsate like a heartbeat?
You’re usually feeling a normal artery close to the skin, especially when lying still or anxious. Worry only with pain, swelling, or one-sided changes.
Is it normal for my leg to have a heartbeat?
Yes, often. Thin people, pregnant people, and anyone lying still can feel arterial pulsation. It’s only abnormal with red flags or a new lump.
Should I worry about a pulsating vein?
Veins don’t normally pulsate; arteries do. A “pulsing vein” is usually an artery underneath. A new lump or hot, tender vein needs evaluation.
What are the warning signs of clogged arteries in legs?
Calf, thigh, or buttock pain with walking that stops at rest is earliest. Other clues: cold foot, pale skin, slow-healing sores, weak pulses.
When should I see a doctor for leg throbbing?
Sudden, severe, or one-sided throbbing with swelling, redness, or breathlessness needs same-day care. Mild throbbing past two to four weeks deserves a check.
When to act
Most leg throbbing is harmless. Most.
The asterisk matters because the conditions that make it dangerous (DVT, pulmonary embolism, acute ischemia) move fast when they move. The cost of getting checked when you didn’t need to is a copay and an hour of your time. The cost of waiting on a clot is much bigger.
If your throb is mild and matches one of the benign patterns above, conservative care will probably handle it. If anything in the triage section earlier describes you, stop reading and call.
For everything in between, a vascular ultrasound is one of the most useful 30 minutes you’ll spend. Most insurance covers it. The peace of mind alone is worth the visit.
Read Next: Unlocking Leg Health: Exercise’s Vital Role Explained